Vibrio vulnificus
| Vibrio vulnificus | |
|---|---|
| |
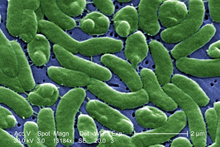
| False-color SEM image of Vibrio vulnificus | |
| Scientific classification | |
| Domain: | Bacteria |
| Phylum: | Pseudomonadota |
| Class: | Gammaproteobacteria |
| Order: | Vibrionales |
| Family: | Vibrionaceae |
| Genus: | Vibrio |
| Species: | V. vulnificus
|
| Binomial name | |
| Vibrio vulnificus | |
| Synonyms | |
| |
Vibrio vulnificus is a species of Gram-negative, motile, curved rod-shaped (vibrio), pathogenic bacteria of the genus Vibrio. Present in marine environments such as estuaries, brackish ponds, or coastal areas, V. vulnificus is related to V. cholerae, the causative agent of cholera.[3] At least one strain of V. vulnificus is bioluminescent.[4] Increasing seasonal ocean temperatures and low-salt marine environments like estuaries favor a greater concentration of Vibrio within filter-feeding shellfish; V. vulnificus infections in the Eastern United States have increased eightfold from 1988–2018.
Infection with V. vulnificus leads to rapidly expanding skin infections by entering a wound causing cellulitis or even sepsis.[5]: 279 V. vulnificus is also a source of foodborne illness. It was first isolated as a source of disease in 1976.[6]
Strains
[edit]Vibrio vulnificus is a species of Gram-negative, motile, curved rod-shaped (bacillus), pathogenic bacteria of the genus Vibrio. Present in marine environments such as estuaries, brackish ponds, or coastal areas, V. vulnificus is related to V. cholerae, the causative agent of cholera.[7] The most harmful strains of V. vulnificus documented have been observed in three different forms. The first is in an anti-phagocytic polysaccharide capsule that protects the bacteria. By encapsulating the bacteria, phagocytosis and opsonization can not occur, thus allowing the bacteria to continue throughout the organism it is in. The second way that V. vulnificus has been most harmful is with some of the toxins that it creates. These toxins are not part of the infection that V. vulnificus causes but instead they are part of a secondary infection in the gastrointestinal tract that most certainly will lead to systemic infection. Lastly, V. vulnificus has been seen to cause more harm in patients who have higher levels of iron.[8]
Genome Size
[edit]The genome size of V. vulnificus is approximately 5.3 Mbp. The genome is organized into two circular replicons, similar to that of V. cholerae, which also has a large and small chromosome. However, the genome of V. vulnificus is at least one megabase bigger.[9][10][11][12]
Natural transformation
[edit]Natural transformation is a bacterial adaptation for DNA transfer between individual cells. V. vulnificus was found to become naturally transformable during growth on chitin in the form of crab shells.[13] The ability to now carry out transformation experiments in the laboratory should facilitate molecular genetic analysis of this opportunistic pathogen.[citation needed]
Signs and symptoms
[edit]Vibrio vulnificus is an extremely virulent bacterium that can cause three types of infections:
- Acute gastroenteritis from eating raw or undercooked shellfish: V. vulnificus causes an infection often incurred after eating seafood, especially raw or undercooked oysters. It does not alter the appearance, taste, or odor of oysters.[14] Symptoms include vomiting, diarrhea, and abdominal pain.
- Necrotizing wound infections can occur in injured skin exposed to contaminated marine water. V. vulnificus bacteria can enter the body through open wounds when swimming or wading in infected waters,[3] or by puncture wounds from the spines of fishes such as stingrays. People may develop a blistering dermatitis sometimes mistaken for pemphigus or pemphigoid.
- Invasive sepsis can occur after eating raw or undercooked shellfish, especially oysters. V. vulnificus is 80 times more likely to spread into the bloodstream in people with compromised immune systems, especially those with chronic liver disease. When this happens, severe symptoms including blistering skin lesions and septic shock can sometimes lead to death.[15][16] This severe infection may occur regardless of whether the infection began from contaminated food or an open wound.[16]
Among healthy people, ingestion of V. vulnificus can cause vomiting, diarrhea, and abdominal pain. In someone with a compromised immune system, particularly those with chronic liver disease, it can infect the bloodstream, causing a severe and life-threatening illness characterized by fever and chills, decreased blood pressure (septic shock), and blistering skin lesions. While men have been shown to be more at risk from this infection than women, co-morbidities such as alcoholic cirrhosis and diseases affecting the endocrine system (diabetes, rheumatoid arthritis, etc.) put a person far more at risk to develop infection from V. vulnificus.[8]
Pathogenesis
[edit]Capsule: V. vulnificus has a capsule, made of polysaccharides, and is thought to protect against phagocytosis.[17] The capsule also aids the bacteria in escaping opsonization.[18] Different strains of the bacteria are capable of shifting through the unencapsulated and encapsulated forms. Mouse models have shown that the unencapsulated forms are avirulent. These same strains however, are shown to have a higher predisposition to shift to the virulent encapsulated form when taken up by oysters.[19]
Endotoxin: Like all gram-negative bacteria, V. vulnificus has LPS (lipopolysaccharide as the major component of its outer membrane). However, the LPS the bacteria produces isn't as efficient at triggering the immune system's release of tumor necrosis factor (TNF) alpha and other cytokines that produce shock syndromes. The capsular proteins the bacteria express however, are capable of producing an immune response contributing to shock syndrome.[20]
Exotoxin: V. vulnificus produces a number of extracellular toxins such as metalloprotease VvpE, cytolysin/hemolysin VvhA, and the multifunctional autoprocessing repeats-in-toxins (MARTX) toxin. While the VvhA and MARTX toxin are factors in the bacteria's virulence, in vivo studies in mice suggest that the MARTX toxin is more responsible for bacterial dissemination from the intestine to produce sepsis.[21][22]
Iron: Growth of V. vulnificus is dependent on the amount of iron that is accessible to the bacteria.[23][24][25][26] The observed association of the infection with liver disease (associated with increased serum iron) might be due to the capability of more virulent strains to capture iron bound to transferrin.[17]
Type IV Pilus: V. vulnificus has genes that encode for the biosynthesis of a type IV pilus. These genes have been located on the large chromosome and may help V. vulnificus adhere to host cells and with motility. [9]
Treatment
[edit]Vibrio vulnificus wound infections have a mortality rate around 25%. In people in whom the infection worsens into sepsis, typically following ingestion, the mortality rate rises to 50%. The majority of these people die within the first 48 hours of infection. The optimal treatment is not known, but in one retrospective study of 93 people in Taiwan, use of a third-generation cephalosporin and a tetracycline (e.g., ceftriaxone and doxycycline, respectively) was associated with an improved outcome.[27] Prospective clinical trials are needed to confirm this finding, but in vitro data support the suggestion that this combination is synergistic against V. vulnificus. Likewise, the American Medical Association and the Centers for Disease Control and Prevention (CDC) recommend treating the person with a quinolone or intravenous doxycycline with ceftazidime. The first successful documented treatment of fulminant V. vulnificus sepsis was in 1995. Treatment was ceftazidime and intravenous (IV) ciprofloxacin and IV doxycycline, which proved successful. Prevention of secondary infections from respiratory failure and acute renal failure is crucial. Key to the diagnosis and treatment were the early recognition of bullae in an immunocompromised person with liver cirrhosis and oyster ingestion within the previous 48 hours, and the request by the physician for STAT Gram staining and blood cultures for V. vulnificus.[28] Amputation of limbs may be required.[29] Vibrio vulnificus often causes large, disfiguring ulcers that require extensive debridement or even amputation.[citation needed]
Prognosis
[edit]Vibrio vulnificus is the most common cause of death due to seafood in the United States, causing over 95% of deaths that are known to have occurred due to ingested seafood. If treatment with tetracycline or other cephalosporin antibiotics is initiated at the onset of symptoms and the full course followed, patients generally experience no long term effects.[30]
The worst prognosis is in those people arriving at hospital in a state of shock. Total mortality in treated people (ingestion and wound) is around 33%.[27]
People especially vulnerable are those with liver disease (especially cirrhosis and hepatitis) or immunocompromised states (some kinds of cancer, bone marrow suppression, HIV, diabetes, etc.). With these cases, V. vulnificus usually enters the bloodstream, where it may cause fever and chills, septic shock (with sharply decreased blood pressure), and blistering skin lesions.[31] About half of those who contract blood infections die.
The consumption of contaminated raw oysters in those with chronic liver disease causes primary septicemia with a mortality rate of over 50%. Exposure of wounds to contaminated seawater or handling of contaminated seafood products causes infections with a mortality rate of about 25%.[9][32][33]
Vibrio vulnificus infections also disproportionately affect males; 85% of those developing endotoxic shock from the bacteria are male. Females having had an oophorectomy experienced increased mortality rates, as estrogen has been shown experimentally to have a protective effect against V. vulnificus.[34]
Epidemiology
[edit]Vibrio vulnificus is commonly found in the Gulf of Mexico, where more than a dozen people have died from the infection since 1990.[35] Most deaths at that time were occurring due to fulminant sepsis, either in the area of oyster harvest and ingestion, or in tourists returning home. Lack of disease recognition, and also of the risk factors, presentation, and cause, were and are major obstacles to good outcome and recovery.[citation needed]
Increasing seasonal temperatures and decreasing salinity levels seem to favor a greater concentration of Vibrio within filter-feeding shellfish of the U.S. Atlantic seaboard and the Gulf of Mexico, especially oysters (Crassostrea virginica). Scientists have frequently demonstrated the presence of V. vulnificus in the gut of oysters and other shellfish and in the intestines of fish that inhabit oyster reefs. The vast majority of people who develop sepsis from V. vulnificus became ill after they ate raw oysters; most of these cases have been men.[36]
According to the CDC, V. vulnificus infections in the Eastern United States increased eightfold from 1988–2018 and the border of where these infections occur has migrated 48 km Northward each year. In July–August 2023, Connecticut, New York, and North Carolina, reported severe and fatal V. vulnificus infections.[37]
Research
[edit]While the treatment for V. vulnificus can be as straightforward as making the rapid choice of appropriate antibiotics, there have been cases in which the genes mutated, thus rendering antibiotics ineffective. While looking for an answer to this problem, researchers found that one way to stop the infection from spreading is to again mutate the bacteria. This mutation happens on the flagellum of the bacteria. When injected with flgC and flgE (two genes in the flagella that cause the mutation), the flagellum no longer function properly. When unable to move normally, the bacteria is no longer able to spread toxins through the body, thus decreasing the effect that V. vulnificus has on the body systemically.[38]
History
[edit]The pathogen was first isolated in 1976 from a series of blood culture samples submitted to the CDC in Atlanta.[6] It was described as a "lactose-positive vibrio".[6] It was initially given the name Beneckea vulnifica[1], and then finally the name Vibrio vulnificus by J. J. Farmer in 1979.[2]
In 2005, health officials clearly identified strains of V. vulnificus infections among evacuees from New Orleans due to the flooding there caused by Hurricane Katrina.[39]
In 2015, eight cases of V. vulnificus infection were reported in Florida, with two resulting in death.[40]
In 2022, following Hurricane Ian, Lee County, Florida, saw a sharp rise in infections and deaths from V. vulnificus. By October 18, 2022, four deaths and 29 illnesses had been recorded since landfall of the hurricane in late September.[41][42]
In 2023, it was reported that a 40-year-old woman from California had been infected by Vibrio vulnificus after eating undercooked fish (tilapia). She had her four limbs removed in order to save her life.[43] However, upon further investigation, local public health officials reported no evidence of V. vulnificus infection in her case. [44]
See also
[edit]References
[edit]- ^ a b Reichelt JL, Baumann P, Baumann L (October 1976). "Study of genetic relationships among marine species of the genera Beneckea and Photobacterium by means of in vitro DNA/DNA hybridization". Arch. Microbiol. 110 (1): 101–20. Bibcode:1976ArMic.110..101R. doi:10.1007/bf00416975. PMID 1015934. S2CID 23759213.
- ^ a b Farmer JJ (October 1979). "Vibrio ("Beneckea") vulnificus, the bacterium associated with sepsis, septicaemia, and the sea". Lancet. 314 (8148): 903. doi:10.1016/S0140-6736(79)92715-6. PMID 90993. S2CID 34979437.
- ^ a b Oliver JD (2005). "Wound infections caused by Vibrio vulnificus and other marine bacteria". Epidemiol Infect. 133 (3): 383–91. doi:10.1017/S0950268805003894. PMC 2870261. PMID 15962544.
- ^ ""Glowing" Seafood?"" (PDF). U.S. Food And Drug Administration Seafood Products Research Center. Archived (PDF) from the original on 2020-11-27. Retrieved 2021-03-09.
- ^ James, William D.; Berger, Timothy G. (2006). Andrews' Diseases of the Skin: Clinical Dermatology. Saunders Elsevier. ISBN 978-0-7216-2921-6.
- ^ a b c Hollis DG, Weaver RE, Baker CN, Thornsberry C (April 1976). "Halophilic Vibrio species isolated from blood cultures". J. Clin. Microbiol. 3 (4): 425–31. doi:10.1128/jcm.3.4.425-431.1976. PMC 274318. PMID 1262454.
- ^ Oliver JD, Kaper J (2001). Vibrio species. pp. 263-300 In: Food Microbiology: Fundamentals and Frontiers. (Doyle MP et al., editors) (2nd ed.). ASM Press. ISBN 978-1-55581-117-4.
- ^ a b "UpToDate". www.uptodate.com. Archived from the original on 2019-06-21. Retrieved 2019-06-21.
- ^ a b c Chen, C.Y.; Wu, K.M.; Chang, Y.C.; Chang, C.H.; Tsai, H.C.; Liao, T.L.; Liu, Y.M.; Chen, H.J.; Shen, A.B.; Li, J.C.; Su, T.L.; Shao, C.P.; Lee, C.T.; Hor, L.I.; Tsai, S.F. (2003). "Comparative genome analysis of Vibrio vulnificus, a marine pathogen". Genome Research. 13 (12): 2577–2587. doi:10.1101/gr.1295503. PMC 403799. PMID 14656965.
- ^ Yamaichi, Y.; Iida, T.; Park, K.S.; Yamamoto, K.; Honda, T. (1999). "Physical and genetic map of the genome of Vibrio parahaemolyticus: presence of two chromosomes in Vibrio species". Molecular Microbiology. 31 (5): 1513–1521. doi:10.1046/j.1365-2958.1999.01296.x. PMID 10200969 – via NCBI.
- ^ Trucksis, M.; Michalski, J.; Deng, Y.K.; Kaper, J.B. (1998). "The Vibrio cholerae genome contains two unique circular chromosomes". Proceedings of the National Academy of Sciences of the United States of America. 95 (24): 14464–14469. Bibcode:1998PNAS...9514464T. doi:10.1073/pnas.95.24.14464. PMC 24396. PMID 9826723.
- ^ Heidelberg, J.F.; Eisen, J.A.; Nelson, W.C.; Clayton, R.A.; Gwinn, M.L.; Dodson, R.J.; Haft, D.H.; Hickey, E.K.; Peterson, J.D.; Umayam, L.; Gill, S.R.; Nelson, K.E.; Read, T.D.; Tettelin, H.; Richardson, D. (2000). "DNA sequence of both chromosomes of the cholera pathogen Vibrio cholerae". Nature. 406 (6795): 477–483. doi:10.1038/35020000. PMC 8288016. PMID 10952301.
- ^ Gulig PA, Tucker MS, Thiaville PC, Joseph JL, Brown RN (2009). "USER friendly cloning coupled with chitin-based natural transformation enables rapid mutagenesis of Vibrio vulnificus". Appl. Environ. Microbiol. 75 (15): 4936–49. Bibcode:2009ApEnM..75.4936G. doi:10.1128/AEM.02564-08. PMC 2725515. PMID 19502446.
- ^ "Vibrio Species Causing Vibriosis". Centers for Disease Control. Archived from the original on June 16, 2017. Retrieved June 5, 2017.
- ^ "Vibrio vulnificus". NCBI Genome Project. Archived from the original on 2021-09-07. Retrieved 2005-09-01.
- ^ a b "Vibrio Species Causing Vibriosis - Questions and Answers". Centers for Disease Control. Archived from the original on June 7, 2017. Retrieved June 5, 2017.
- ^ a b Oxford handbook of Infect Dis and Microbiol, 2009
- ^ Wright, A. C.; Simpson, L. M.; Oliver, J. D.; Morris, J. G. (June 1990). "Phenotypic evaluation of acapsular transposon mutants of Vibrio vulnificus". Infection and Immunity. 58 (6): 1769–1773. doi:10.1128/IAI.58.6.1769-1773.1990. ISSN 0019-9567. PMC 258721. PMID 2160432.
- ^ Srivastava, Milan; Tucker, Matthew S.; Gulig, Paul A.; Wright, Anita C. (August 2009). "Phase variation, capsular polysaccharide, pilus and flagella contribute to uptake of Vibrio vulnificus by the Eastern oyster ( Crassostrea virginica )". Environmental Microbiology. 11 (8): 1934–1944. Bibcode:2009EnvMi..11.1934S. doi:10.1111/j.1462-2920.2009.01916.x. PMID 19689704.
- ^ Powell, J. L.; Wright, A. C.; Wasserman, S. S.; Hone, D. M.; Morris, J. G. (September 1997). "Release of tumor necrosis factor alpha in response to Vibrio vulnificus capsular polysaccharide in in vivo and in vitro models". Infection and Immunity. 65 (9): 3713–3718. doi:10.1128/IAI.65.9.3713-3718.1997. ISSN 0019-9567. PMC 175529. PMID 9284142.
- ^ Baker-Austin, Craig; Oliver, James D. (February 2018). "Vibrio vulnificus: new insights into a deadly opportunistic pathogen". Environmental Microbiology. 20 (2): 423–430. Bibcode:2018EnvMi..20..423B. doi:10.1111/1462-2920.13955. ISSN 1462-2920. PMID 29027375.
- ^ Gavin, Hannah E.; Satchell, Karla J. F. (2019-02-23). "RRSP and RID Effector Domains Dominate the Virulence Impact of Vibrio vulnificus MARTX Toxin". The Journal of Infectious Diseases. 219 (6): 889–897. doi:10.1093/infdis/jiy590. ISSN 1537-6613. PMC 6386806. PMID 30289477.
- ^ Brennt, C. E.; Wright, A. C.; Dutta, S. K.; Morris, J. G. (November 1991). "Growth of Vibrio vulnificus in serum from alcoholics: association with high transferrin iron saturation". The Journal of Infectious Diseases. 164 (5): 1030–1032. doi:10.1093/infdis/164.5.1030. ISSN 0022-1899. PMID 1940460.
- ^ Kim, Choon-Mee; Park, Ra-Young; Choi, Mi-Hwa; Sun, Hui-Yu; Shin, Sung-Heui (2007-01-01). "Ferrophilic characteristics of Vibrio vulnificus and potential usefulness of iron chelation therapy". The Journal of Infectious Diseases. 195 (1): 90–98. doi:10.1086/509822. ISSN 0022-1899. PMID 17152012.
- ^ Kim, Choon-Mee; Park, Yong-Jin; Shin, Sung-Heui (2007-11-15). "A widespread deferoxamine-mediated iron-uptake system in Vibrio vulnificus". The Journal of Infectious Diseases. 196 (10): 1537–1545. doi:10.1086/523108. ISSN 0022-1899. PMID 18008234.
- ^ Mura, C.; Le Gac, G.; Scotet, V.; Raguenes, O.; Mercier, A. Y.; Férec, C. (2001). "Variation of iron loading expression in C282Y homozygous haemochromatosis probands and sib pairs". Journal of Medical Genetics. 38 (9): 632–636. doi:10.1136/jmg.38.9.632. PMC 1734933. PMID 11565552.
- ^ a b Liu JW, Lee IK, Tang HJ, et al. (2006). "Prognostic factors and antibiotics in Vibrio vulnificus septicemia". Archives of Internal Medicine. 166 (19): 2117–23. doi:10.1001/archinte.166.19.2117. PMID 17060542.
- ^ "Vibrio vulnificus fact sheet" (PDF). issc.org. Archived from the original (PDF) on 21 July 2016. Retrieved August 1, 2016.
- ^ "Learn how to prevent a Vibrio wound infection". Centers for Disease Control and Prevention. November 1, 2022. Retrieved September 20, 2023.
- ^ "Vibrio Vulnificus Infection: Background, Pathophysiology, Etiology". Medscape. 2019-07-01. Archived from the original on 2021-04-16. Retrieved 19 October 2022.
- ^ Oliver JD, Kaper J (2005). Vibrio vulnificus. In: Oceans and Health: Pathogens in the Marine Environment. (Belken SS, Colwell RR, editors) (2nd ed.). Springer Science. ISBN 978-0-387-23708-4.
- ^ Blake, P.A.; Merson, M.H.; Weaver, R.E.; Hollis, D.G.; Heublein, P.C. (1979). "Disease caused by a marine Vibrio. Clinical characteristics and epidemiology". The New England Journal of Medicine. 300 (1): 1–5. doi:10.1056/NEJM197901043000101. PMID 758155 – via NCBI.
- ^ Hlady, W.G.; Klontz, K.C. (1996). "The epidemiology of Vibrio infections in Florida, 1981-1993". The Journal of Infectious Diseases. 173 (5): 1176–1183. doi:10.1093/infdis/173.5.1176. PMID 8627070 – via NCBI.
- ^ Merkel SM, Alexander S, Zufall E, Oliver JD, Huet-Hudson YM (2001). "Essential Role for Estrogen in Protection against Vibrio vulnificus-Induced Endotoxic Shock". Infection and Immunity. 69 (10): 6119–22. doi:10.1128/IAI.69.10.6119-6122.2001. PMC 98741. PMID 11553550.
- ^ Flynn, Dan (November 22, 2011). "Still Too Many Raw Oyster Deaths in Gulf States". Food Safety News. Archived from the original on October 9, 2016. Retrieved August 1, 2016.
- ^ Diaz, James H. (May 2014). "Skin and Soft Tissue Infections Following Marine Injuries and Exposures in Travelers". Journal of Travel Medicine. 21 (3): 207–213. doi:10.1111/jtm.12115. ISSN 1195-1982. PMID 24628985.
- ^ CDC Health Alert Network (HAN) - 00497 (2023-09-01). "Severe Vibrio vulnificus Infections in the United States Associated with Warming Coastal Waters". emergency.cdc.gov. Archived from the original on 2023-09-02. Retrieved 2023-09-02.
{{cite web}}: CS1 maint: numeric names: authors list (link) - ^ Oliver, James D.; Jones, Melissa K. (2009-05-01). "Vibrio vulnificus: Disease and Pathogenesis". Infection and Immunity. 77 (5): 1723–1733. doi:10.1128/IAI.01046-08. ISSN 0019-9567. PMC 2681776. PMID 19255188.
- ^ Gold, Scott (September 6, 2005). "Newest Peril from Flooding Is Disease". Los Angeles Times.
- ^ Katy Galimberti (June 18, 2015). "Flesh-Eating Bacteria Kills Two in Florida as Water Temperatures Rise". msn.com. Archived from the original on August 5, 2016. Retrieved August 1, 2016.
- ^ Matza, Max (2022-10-19). "Florida flesh-eating illness cases spike after Hurricane Ian". BBC News. Archived from the original on 2022-10-18. Retrieved 2022-10-18.
- ^ Melissa Montoya; Amy Oshier (October 14, 2022). "Michigan man dies from bacteria while helping in Ian recovery". Wink News, Fort Meyers Broadcasting Company. Archived from the original on 21 October 2022. Retrieved 21 October 2022.
- ^ Alund, Natalie Neysa (2023-09-19). "California mother's limbs amputated after flesh-eating bacteria infection linked to fish: Report". USA Today. Archived from the original on 2023-09-21. Retrieved 2023-09-20.
- ^ O'Neill, Maggie (2023-09-21). "Health officials cast doubt on report of woman who had limbs amputated after bacterial infection from tilapia". Independent. Archived from the original on 2023-10-03. Retrieved 2023-10-19.
